Understanding Your 12-Week Scan
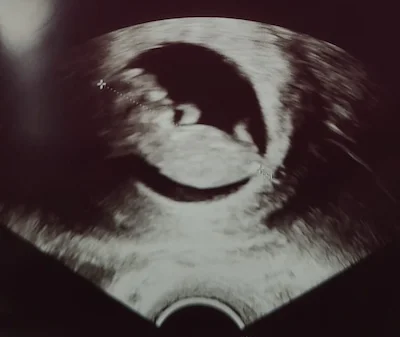
Celebrate the first big milestone of your journey as you see your baby’s growth and prepare for the exciting road ahead.
The 12-week scan is one of the most anticipated moments in early pregnancy, marking an important milestone in your journey to parenthood. Also known as the dating scan or nuchal translucency scan, this routine ultrasound provides crucial information about your baby's development and helps establish your due date. Understanding what happens during this scan can help you feel more prepared and confident as you approach this exciting appointment.
What is the 12-week scan?
The 12-week scan is typically performed between 11 and 14 weeks of pregnancy, with the optimal timing being between 11 weeks 2 days and 13 weeks 6 days. This scan serves multiple important purposes and is offered to all pregnant women on the NHS as part of routine antenatal care.
The scan combines two key assessments:
- Dating scan: Confirms how many weeks pregnant you are and calculates your estimated due date
- Nuchal translucency screening: Measures the fluid at the back of your baby's neck to assess the risk of chromosomal conditions
This ultrasound is usually performed abdominally, though occasionally a transvaginal scan may be needed if the baby's position makes it difficult to get clear images. The scan typically takes 15-30 minutes and is conducted by a trained sonographer or doctor.
Why is the 12-week scan important?
The 12-week scan provides essential information that helps guide your pregnancy care. Here is what makes this scan so significant:
Accurate dating
Whilst you may have calculated your due date based on your last menstrual period, the 12-week scan provides a much more accurate estimate. The measurement of your baby's crown-rump length (the distance from the top of the head to the bottom of the spine) gives the most precise dating available. This accurate dating is crucial for:
- Planning future antenatal appointments and scans
- Determining the optimal timing for screening tests
- Assessing whether your baby is growing appropriately at later scans
- Planning your maternity leave and preparing for birth
Viability assessment
The scan confirms that your baby has a heartbeat and is developing normally. By 12 weeks, all major organs have formed, and the risk of miscarriage significantly decreases after a normal scan at this stage.
Multiple pregnancy detection
If you are carrying twins, triplets, or more, this scan will identify multiple pregnancies. This information is vital for planning appropriate care, as multiple pregnancies require more frequent monitoring and may need specialist management.
Screening for chromosomal conditions
The nuchal translucency measurement, combined with blood tests, helps assess the risk of conditions such as Down's syndrome, Edwards' syndrome, and Patau's syndrome. This screening gives you information to help make informed decisions about further testing if desired.
What to expect during your scan
Understanding what happens during your 12-week scan can help reduce anxiety and ensure you are well-prepared for this important appointment.
Before the scan
You will typically receive your appointment letter from your GP or midwife, usually scheduled after your booking appointment. Here is how to prepare:
- Timing: Arrive with a moderately full bladder, as this helps provide clearer images of your baby
- Clothing: Wear comfortable, loose-fitting clothes that can be easily lifted to expose your abdomen
- Partner: Most hospitals welcome your partner or a support person to accompany you
- Questions: Prepare any questions you would like to ask about your pregnancy or the scan
During the scan
The sonographer will explain what they are doing throughout the procedure:
- A clear gel is applied to your abdomen to help the ultrasound waves travel
- The sonographer moves a transducer (small handheld device) over your abdomen
- Images of your baby appear on the screen, and you will be able to see your baby for the first time
- Various measurements are taken, including the crown-rump length and nuchal translucency
- The sonographer checks your baby's basic anatomy and looks for any obvious abnormalities
- Photos are usually provided as keepsakes
Remember: The sonographer needs to concentrate during the scan, so there may be periods of silence whilst they take measurements. This is completely normal and does not indicate any problems.
Key measurements and checks
During your 12-week scan, several important measurements and assessments are made:
Crown-rump length (crl)
This is the most important measurement for dating your pregnancy. The sonographer measures from the top of your baby's head to their bottom. At 12 weeks, this measurement is typically around 5-6 centimetres.
Nuchal translucency (nt)
This measures the thickness of fluid at the back of your baby's neck. A measurement of less than 3.5mm is considered normal, though this varies slightly depending on the exact gestational age. This measurement, combined with blood test results, helps calculate the risk of chromosomal conditions.
Heartbeat
The sonographer will check that your baby's heart is beating normally. At 12 weeks, the heart rate is typically between 120-180 beats per minute.
Basic anatomy
Whilst detailed anatomy assessment occurs at the 20-week scan, the sonographer will check basic structures including:
- Head shape and brain structures
- Spine alignment
- Limb presence and basic structure
- Abdominal wall closure
- Placental position
Combined screening test
The 12-week scan is often combined with blood tests to form the "combined screening test" for chromosomal conditions. This screening is optional, and you will have the opportunity to discuss it with your midwife before deciding whether to proceed.
What the blood test measures
The blood test typically measures two hormones:
- Free beta-hCG: Human chorionic gonadotrophin
- PAPP-A: Pregnancy-associated plasma protein A
Understanding your results
The results are given as a risk ratio, such as 1 in 1,000 or 1 in 150. This means that out of women with the same risk, one would be expected to have a baby with the condition. Results are typically categorised as:
- Lower risk: 1 in 150 or lower risk
- Higher risk: Greater than 1 in 150
It is important to understand that this is a screening test, not a diagnostic test. A higher-risk result does not mean your baby definitely has a condition, just that further testing might be offered.
What can and cannot be detected
Understanding the limitations of the 12-week scan helps set appropriate expectations:
What can be detected
- Accurate gestational age and due date
- Number of babies (multiples)
- Heartbeat confirmation
- Basic anatomical structures
- Some major structural abnormalities
- Risk assessment for chromosomal conditions (when combined with blood tests)
- Placental location
- Some pregnancy complications
What cannot be detected
- Detailed organ structure (this comes at the 20-week scan)
- Baby's gender (though some private scans may attempt this)
- All birth defects or genetic conditions
- Future pregnancy complications
- Learning disabilities or developmental delays
Important: No scan can guarantee that your baby is completely healthy. The 12-week scan provides valuable information, but it is part of ongoing monitoring throughout your pregnancy.
After your scan
Following your 12-week scan, several things typically happen:
Immediate results
The sonographer will usually be able to tell you immediately if everything appears normal with your baby's development. They will provide you with your new estimated due date if it differs from your original calculation.
Screening results
If you have had the combined screening test, results are typically available within a few days to two weeks. You will usually receive these through your midwife or GP, who can explain what they mean and discuss any next steps if needed.
Next appointments
Your midwife will schedule your next antenatal appointment, typically around 16 weeks, and your anomaly scan at around 20 weeks. The 12-week scan results help determine the timing and frequency of future care.
Sharing your news
Many couples choose to share their pregnancy news publicly after the 12-week scan, as the risk of miscarriage significantly decreases after this point. This is entirely your personal choice and there is no right or wrong time to tell family and friends.
When concerns arise
Whilst most 12-week scans show normal development, sometimes concerns may be identified. Understanding how these are handled can help reduce anxiety:
Technical difficulties
Sometimes, clear images cannot be obtained due to:
- Baby's position
- Maternal body habitus
- Bladder fullness
In these cases, you may be asked to return for another scan in a week or two, or a transvaginal scan might be offered.
Measurement concerns
If measurements suggest your baby is smaller or larger than expected, or if the nuchal translucency is increased, you will be referred for specialist consultation. Remember that many babies who have unusual measurements are completely healthy.
Structural concerns
If any structural abnormalities are suspected, you will be referred to a specialist fetal medicine unit for detailed assessment and counselling about options.
Frequently asked questions
The 12-week scan is a routine ultrasound offered to all pregnant women, typically performed between 11 weeks 2 days and 13 weeks 6 days. It is often called the dating scan because it provides the most accurate estimate of your due date. It also measures the nuchal translucency, fluid at the back of the baby's neck, to assess the risk of certain chromosomal conditions. The scan usually takes between 15 and 30 minutes.
Arrive with a moderately full bladder. This pushes the uterus up and out of the pelvis, making the baby easier to see on the scan. Wear a two-piece outfit such as a top and trousers so your abdomen can be easily accessed. The sonographer will apply a clear, cool gel to your tummy and move a handheld transducer over the skin to create images of your baby on a monitor.
The key measurement is the Crown-Rump Length (CRL), the distance from the top of the head to the bottom of the spine, usually around 5–6cm at this stage, which establishes your due date more accurately than using your last period alone. The sonographer also measures the nuchal translucency, the fluid-filled space at the back of the baby's neck, where a measurement under 3.5mm is typically considered lower risk. Basic anatomy checks include the skull, brain structure, spine, and abdominal wall. The baby's heartbeat is confirmed and any multiple pregnancy is identified at this stage.
The combined test is an optional screening that uses your scan measurements alongside a blood test to assess the risk of Down's syndrome (Trisomy 21), Edwards' syndrome (Trisomy 18), and Patau's syndrome (Trisomy 13). Results are given as a risk ratio. For example, 1 in 5,000. A higher risk result (usually greater than 1 in 150) does not mean a condition is present, but it does mean further diagnostic testing such as amniocentesis may be offered to give a definitive answer.
If the baby is lying in a position that makes it difficult to get clear measurements, the sonographer may suggest a transvaginal scan using a small internal probe. This is very common and completely safe. You may also be asked to walk around or cough to encourage the baby to move into a better position before trying again.
It is usually too early at 12 weeks to accurately determine the baby's sex, so most sonographers will not attempt to do so at this stage. A full anomaly scan checking the heart, kidneys, and other organs in detail happens later at 20 weeks. This is also when the sex can more reliably be identified if you wish to find out. The 12-week scan cannot detect non-physical conditions such as learning disabilities or autism.
A healthy 12-week scan is a very reassuring milestone. After it, the risk of miscarriage decreases significantly. The scan confirms the baby has a steady heartbeat and is developing within the uterus, establishes your accurate due date, and provides the clinical data that shapes the rest of your pregnancy care. For many parents it is also the moment the pregnancy becomes visually real for the first time.
Final thoughts
The 12-week scan represents a significant milestone in your pregnancy journey, providing reassurance about your baby's development and helping you plan for the months ahead. Most scans show healthy, normally developing babies, allowing you to progress through your pregnancy with confidence.
Understanding what to expect from this scan can help you feel more prepared and enable you to make the most of this special opportunity to see your baby for the first time. The information gathered helps ensure you receive the most appropriate care throughout your pregnancy.
If you have specific concerns about your pregnancy or would prefer the personal attention and detailed care that comes with private antenatal monitoring, my team and I offer comprehensive pregnancy care in a comfortable, unhurried environment. We take the time to discuss your scan results thoroughly and provide the individualised support you deserve during this important time.
